Dr. Di Iorio understands that comprehensive vein treatment can truly improve a patient’s quality of life. As a result, he offers a variety of treatment options that are both effective and minimally invasive. In mild cases of venous disease, a conservative treatment plan may be suitable, such as exercise and the use of compression stockings. However, since venous disease is progressive, many patients benefit from the direct treatment of their condition through minimally invasive office based procedures that have little to no down time.
Diagnosis:
Diagnosis begins with a thorough examination of your legs followed by a venous ultrasound. Ultrasound allows us to diagnose and target the source of vein problems, giving a clear picture of how the veins look and are functioning. A quality ultrasound performed by a trained professional and interpreted by a qualified physician is vital to determine if vein disease is present or not. Among his many certifications, Dr. Di Iorio’s training and board certification in diagnostic radiology, along with his multiple advanced ultrasound certifications, ensures that you will receive the most complete examination and accurate diagnosis.
Vein treatments:
At South Austin Vein Center, Dr. Di Iorio performs today’s most advanced, minimally invasive vein treatments to end your vein pain and suffering at the source. After a comprehensive examination and a diagnostic ultrasound of your veins, Dr. Di Iorio will determine an individualized treatment plan. This plan may include one or a combination of minimally invasive procedures, including radiofrequency ablation, ambulatory phlebectomy, and sclerotherapy.
Endovenous Ablation Procedures:
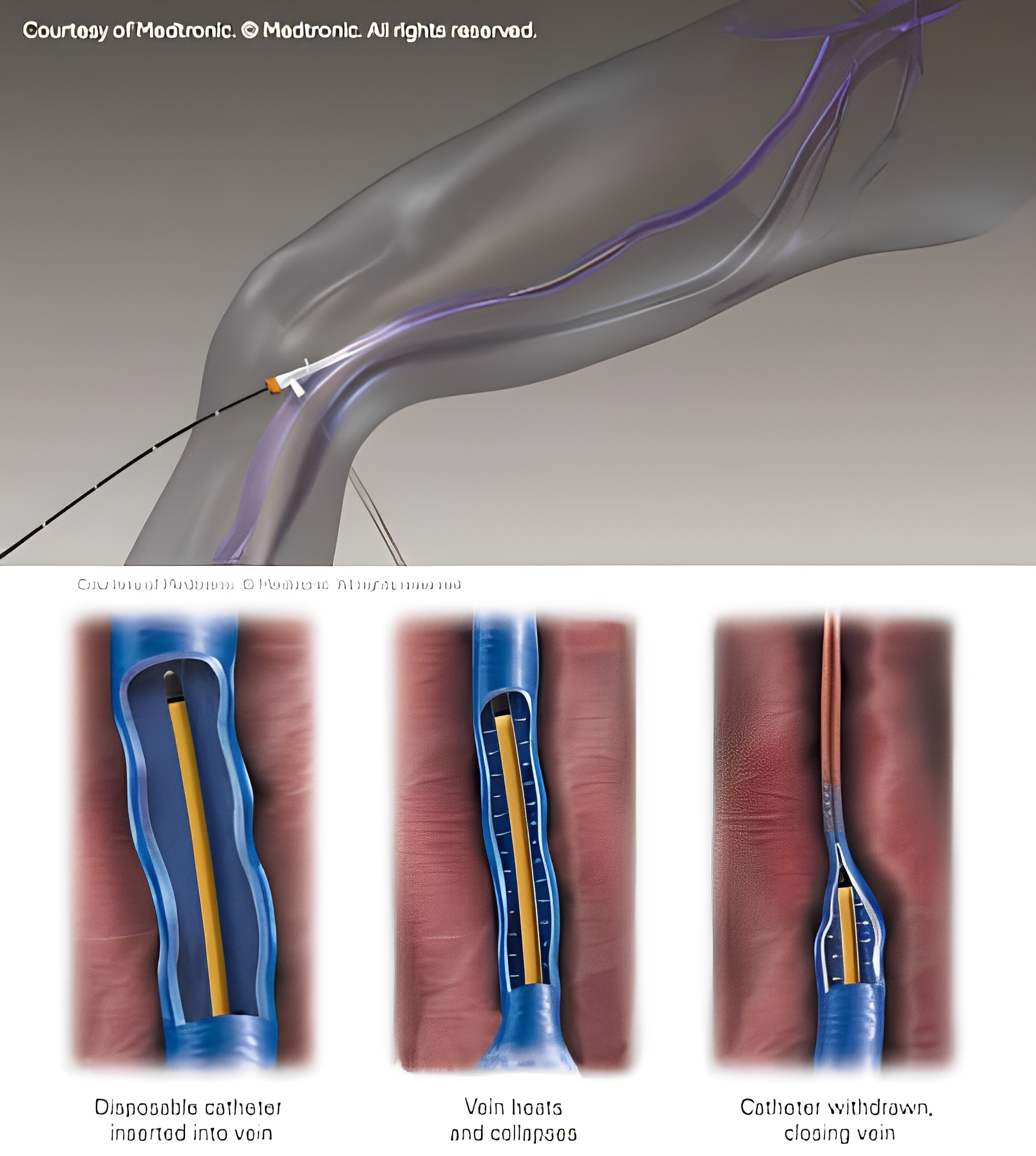
Endovenous radiofrequency ablation (RFA) is a minimally invasive, in-office treatment alternative to surgical stripping. Instead of removing the diseased vein, it is sealed closed in place with heat. The skin over the vein is numbed with local anesthetic and under direct US guidance, a small catheter is inserted through a needle stick into the damaged vein. A dilute local anesthetic is then administered around the vein. The tiny catheter, powered by radiofrequency energy is turned on and slowly pulled back and out of the body sealing the vein closed. Once the vein is sealed, the body automatically reroutes blood flow through healthier vessels to restore normal circulation. Following the procedure, a compression stocking is placed on the treated leg to aid healing. The procedure takes less than 30 minutes and the use of local anesthetic makes the treatment virtually painless. You will be encouraged to walk and resume normal activities immediately following the procedure.
VenaSeal:
VenaSealᵀᴹ is a new minimally invasive treatment, invented by an interventional radiologist, that improves blood flow by sealing a diseased vein with a special medical adhesive.
Traditional thermal energy procedures use heat to close a vein. The intense heat requires a large volume of numbing medicine, called tumescent, which is injected through several needle sticks. The injections may cause discomfort during the procedure and bruising after the procedure. Since no heat is used during VenaSealᵀᴹ treatment, tumescent medication is not needed.
The VenaSealᵀᴹ Procedure: After local anesthesia is given at the entry site to numb the area, a small catheter is inserted into the vein to be treated under US guidance. Once the catheter is in place, a small amount of specially formulated medical adhesive is instilled along the course of the vein sealing it closed. After the diseased vein is closed, the body naturally reroutes blood through nearby healthy veins. Compression stockings are usually not needed after the procedure.
Clinical studies have demonstrated that the VenaSealᵀᴹ procedure is safe and effective. The procedure is administered without the use of tumescent anesthesia, avoiding patient discomfort associated with multiple needle sticks and reduces recovery time. Many patients return to normal activity immediately after the procedure.
Varithena®:
Varithena® is a nonsurgical FDA approved microfoam (a mixture of medication and gas) that is used to treat a wide variety of varicose veins.
Treatment involves injecting a small amount of Varithena® through a catheter or small needle into a malfunctioning vein under US guidance. The Varithena® microfoam fills and treats the desired section of the vein. The vein collapses and the microfoam is deactivated. When the malfunctioning vein collapses, blood flow shifts to healthier veins nearby. Over time the closed vein is absorbed by the body.
Treatment with Varithena® does not require any incisions or anesthesia and the procedure usually takes less than an hour. Varithena® can be used to treat a wide range of varicose veins including:
- Tortuous (twisted) veins
- Veins above and below the knee
- Veins with small, medium, and large diameters
- Veins previously treated with other methods
Varithena® has been shown to improve symptoms related to or caused by varicose veins, including heaviness, achiness, swelling, throbbing and itching. In addition, most patients treated with Varithena® experienced improved vein appearance.

Ambulatory Microphlebectomy:
Microphlebectomy is used for large bulging veins that are too large to treat with sclerotherapy and are not straight enough to use radiofrequency ablation on.
Tiny incisions are made next to the vein and sections of vein are removed through these small nicks with special tools. The incisions are so small they leave minimal to no scars. This is performed in the office using only local anesthesia. Generally, normal activities may be resumed after several days.
Ultrasound Guided Sclerotherapy:
Ultrasound guided sclerotherapy is a procedure in which a medication, often mixed with gas to create a foam, is injected into a varicose vein destroying the vein lining and closing the vein. The use of ultrasound allows treatment of diseased veins that cannot be seen because they are below the surface of the skin. Ultrasound is used to find these abnormal veins and guide treatment. Once these veins are closed blood is automatically rerouted through other healthier veins and over time the closed veins are reabsorbed by the body.
Sclerotherapy:
Sclerotherapy is a cosmetic procedure performed to reduce the appearance of and eliminate spider veins and reticular veins (small to medium sized bluish veins). Under direct visualization a tiny needle is used to inject the veins with a medication that irritates the lining of the vein. In response, the veins collapse and over time are reabsorbed. Patients may need one to several sclerotherapy treatment sessions for any vein region. There is usually no “recovery” time after sclerotherapy, and patients can resume their regular activities immediately.
Spider Vein Treatment:
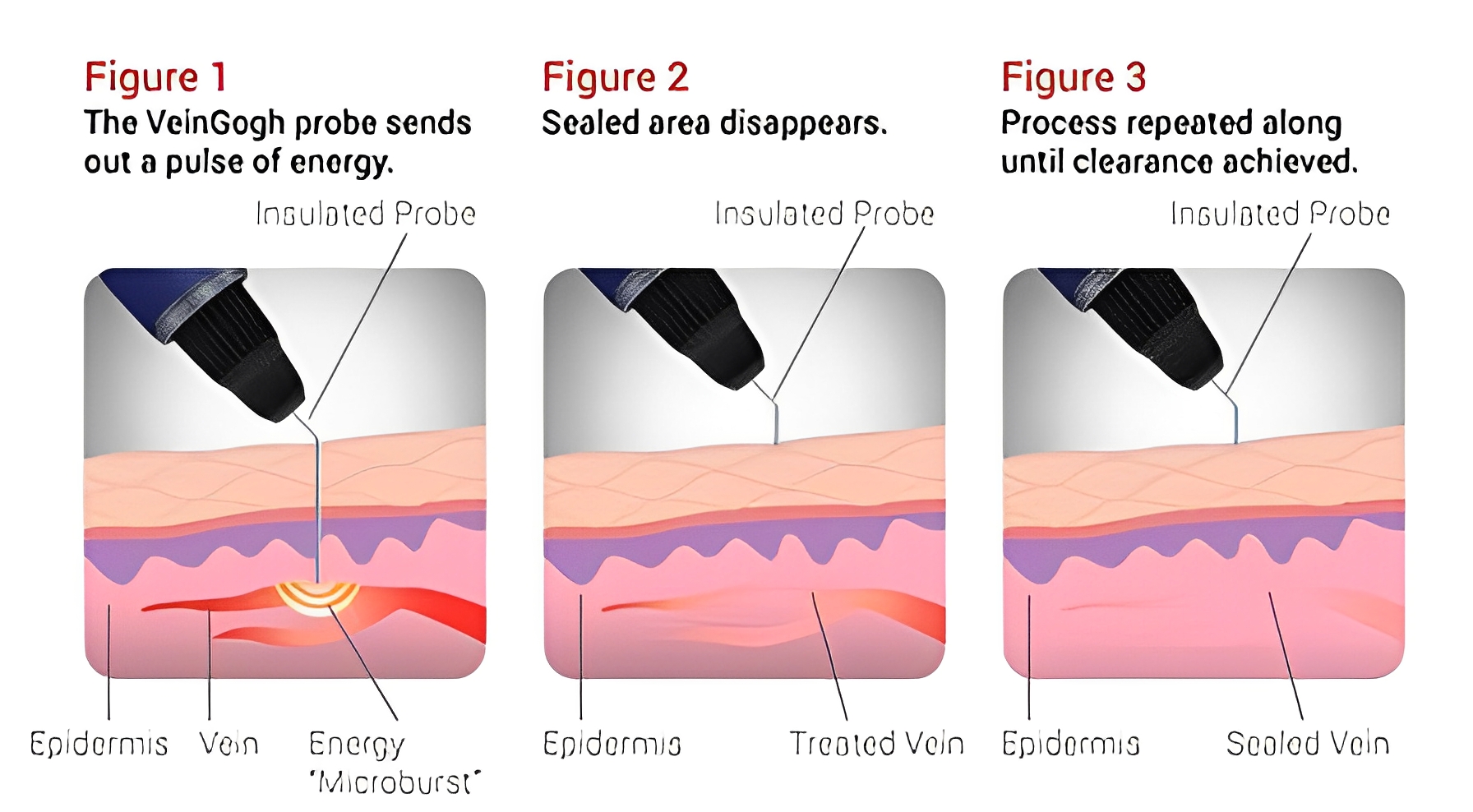
VeinGogh™ is among the newest technologies available for treating telangiectasias, commonly called spider veins. The system uses a technique called ohmic thermolysis to treat unwanted veins by delivering microbursts of high frequency electrical energy via a hair-thin probe. The tiny bursts of energy selectively heat the vein without damaging the overlying skin. The vessel wall collapses and is later absorbed by the body. This technique works best on fine spider veins up to 0.3mm in diameter. Generally, only 1 treatment is needed. However, depending on the specific condition, a follow-up treatment may be necessary. Dr. Di Iorio may use a combination of sclerotherapy and VeinGogh™ for the best overall cosmetic results.
Compression Stockings:
Graduated compression stockings are the mainstay of conservative management and prevention of venous disease. Graduated compression stockings apply a tight pressure around the foot and ankle that gradually decreases as it moves up the leg. This gradient directs the flow of blood in the normal direction, up the leg. Most vein specialist recommend that patients who suffer from varicose veins or have symptoms of venous insufficiency wear compression stockings. Compression stockings are typically prescribed to be worn during active hours when patients are on their feet. Compression stockings are also used following other forms of treatment.

